Alcohol and other drugs
Allied Health
Child and youth health: health professionals
The Best Opportunities in Life – Northern Territory Child and Adolescent Health and Wellbeing Strategic Plan 2018–2028
The Best Opportunities in Life - Child and Adolescent Health and Wellbeing Strategic Plan 2018 -2028 aims to improve health and wellbeing services for young people aged 0-24 years old.
Key focus areas are:
- Health development of children and young adults to ensure they are raised and live in an environment that supports, promotes, protects their physical, emotional, cultural and social development.
- Improved health and wellbeing of young people 0-24 years old, by providing a framework to guide health, housing, education, youth justice, child protection and police services in addressing challenges that currently exist in the Territory.
- Focused and evidence-informed support to ensure children are safe and protected from harm.
The Best Opportunities in Life - Child and Adolescent Health and Wellbeing Strategic Plan 2018–2028
The Best Opportunities in Life: background
The Best Opportunities in Life Strategic Plan was developed through extensive consultation across Northern Territory Government departments, non-government organisations and Aboriginal Community Controlled Health Services. Young Territorians had input through focus groups and a survey to ensure the plan could be developed in a culturally safe, respectful and compassionate manner.
More information on consultation and data informing the strategic plan is available from The Best Opportunities in Life - Child and Adolescent Health and Wellbeing Strategic Plan 2018–2028 Background document
Healthy Pregnancy Healthy Baby Book
The Healthy Pregnancy Healthy Baby booklet is a resource about pregnancy, birth and early parenting for Aboriginal and Torres Strait Islander women and their families.
The Healthy Pregnancy Healthy Baby booklet provides information in plain English about:
- antenatal care and tests
- healthy lifestyle choices in pregnancy
- labour and birth options
- being a new parent.
The original booklet was developed as part of the NT Government's Closing the Gap of Indigenous Disadvantage initiative in 2009 and reviewed in 2019 through the Indigenous Advancement Strategy.
The updated Health Pregnancy Healthy Baby booklet PDF (3.1 MB) is available online.
Contact
Health Improvement
5th Floor, Manunda Place
38 Cavenagh Street
Darwin NT 0811
PO Box 40596,
Casuarina, NT 0811
Phone: (08) 8985 8015
child.health@nt.gov.au
Related information
For more information on child and youth health go to these websites:
- National frameworks and action plans on the Australian Department of Health website
- Raising Children Network on the Australian Parenting website.
Core Clinical Systems Renewal Program (CCSRP)
Introduction
In May 2017, the Northern Territory Government (NTG) provided funding of $259 million to support the Core Clinical Systems Renewal Program (CCSRP). CCSRP will provide a single, secure, Territory–wide, electronic patient record that integrates multiple systems used in NT Health, and will replace current aging clinical systems.
The new system known as Acacia, is being tailored to meet the unique requirements of healthcare in the NT using TrakCare software purchased from InterSystems Corporation.
Acacia is being delivered in a phased approach. Acacia Read-only Electronic Patient Record was rolled out in late 2020. In 2022 the rollout of Acacia 1.0: Patient administration+, replacing CareSys and Jade Care Clinical Booking (JCCB) was rolled out to Katherine Hospital, Gove District Hospital and Top End Renal Services. Over 2023, the rollout of Acacia 1.0: Patient administration+ will continue in remaining NT hospitals and renal dialysis sites.
Next will be the combined rollout of Hospital Care Systems, Acacia 2.0 and Acacia 3.0, supporting medication management, electronic orders and results, and replacing many paper-based workflows, Clinical Work Station and eMMa.
This will be followed by Acacia 4.0, Primary Health Care to support community, urban and remote primary care processes, and Acacia 5.0, the Client and Healthcare Provider Portal, a service information portal for patients and access for authorised external service providers.
Future improvements for patients and clinicians
- Patients will have their healthcare information stored in one secure system NT wide for clinicians to access, reducing the requirement to repeat medical history.
- Patients will experience improved continuity of care as important healthcare information is available at the point of care and added to during their treatment journey and throughout their life.
- Clinicians will have improved access to vital healthcare information as patients transfer from remote areas to NT hospitals.
The CCSRP has a comprehensive and contemporary governance framework and is subject to regular reporting and oversight by the NTG’s Information and Communications Technology Governance Board.
Contact us
If you require further information, email: AcaciaEnquiries.DoH@nt.gov.au
Centre for Disease Control – Public Health Division
The Centre for Disease Control sits within the Public Health Division under the Chief Health Officer. CDC units are located across the five health service regions in the Northern Territory (NT).
Diabetes: Health Professionals
NT Health supports best practice education and care for those living with and at risk of developing diabetes, through the development, implementation and evaluation of evidence-based policies, projects and resources.
NT Health encourages collaboration, information sharing and professional development of health professionals working to prevent diabetes and related chronic conditions, and working with people living with and at risk of developing diabetes across the Northern Territory (NT).
NT Diabetes Network
The NT Diabetes Network was established in February 2018. The Network provides a platform for NT clinicians, researchers and policy makers to work collaboratively and provide clinical leadership to improve the care and health outcomes for people living with and at risk of developing diabetes.
Membership of the NT Diabetes Network and Working Group includes representatives from NT Health, Menzies School of Health Research, NT Primary Health Network, Healthy Living NT, AMSANT and several Aboriginal Community Controlled Health Organisations across the NT.
Information and resources for health professionals
| Resource | Description |
|---|---|
| Screening and management pathways for type 2 diabetes in Aboriginal young people in NT PDF (1.5 MB) | This resource provides clinicians with information on screening and management pathways when working with Aboriginal young people in the NT at risk of developing type 2 diabetes or living with diabetes. Developed by the NT Diabetes Network. |
| Type 2 diabetes remission factsheet PDF (738.6 KB) | This resource provides health professionals in the NT with information on type 2 diabetes remission, and remission suitability and considerations. Developed by the NT Diabetes Network. |
Diabetes and the social determinants of health PPTX (3.2 MB) Video - Diabetes - The link between diabetes and the social determinates of health | This booklet and video were designed for health professionals to share or present to raise awareness of the link between diabetes and the social determinants of health among non-health professionals and organisations. Developed by the NT Diabetes Network. |
| NT Diabetes Summit Roadmap PDF (3.8 MB) | The Roadmap is a summary of the event, outcomes and actions from the NT Diabetes Summit held in November 2022. Developed by the NT Diabetes Summit Partners (NT Health, Menzies School of Health Research, AMSANT, NTPHN, and the Commonwealth Department of Health and Aged Care). |
Consumer diabetes resources
| Resource | Description |
|---|---|
| Type 2 diabetes in young people fact sheet PDF (683.7 KB) | This factsheet was developed for health professionals to use when providing education regarding type 2 diabetes to young people with or at risk of type 2 diabetes, and/or their parents/carers. Developed by the NT Diabetes Network. |
| Healthy Living for Children and Teenagers above a healthy weight PDF (31.9 MB) | This resource has been developed for use with families with children aged 5-18 years who are above a healthy weight. This resource is to be used in conjunction with the Health Professionals Guide – Using the childhood obesity education resource: “Healthy Living for Children and Teenagers above a healthy weight”. Developed by Top End Health Service Public Health Nutritionists. |
| Good food for diabetes from the Healthy Living NT website. | This booklet was developed for health professionals to use when providing education regarding food and diabetes to Aboriginal clients, and/or their families or carers. Developed by Healthy Living NT. |
| Nutrition for diabetes in pregnancy from the Healthy Living NT website. | This resource has been developed for use with pregnant women who have diabetes (type 2 and/or gestational diabetes) Developed by Healthy Living NT. |
| Diabetes in pregnancy videos from the Diabetes across the Lifecourse: Northern Australia Partnership website | These videos have been developed for Aboriginal and Torres Strait Islander women with diabetes during pregnancy. Developed by Menzies School of Health Research, Diabetes across the Lifecourse: Northern Australia Partnership. |
| Diabetes in youth videos from the Diabetes across the Lifecourse: Northern Australia Partnership website | These videos, including a music video and lived experience videos, have been developed for youth with diabetes. Developed by Menzies School of Health Research, Diabetes across the Lifecourse: Northern Australia Partnership. |
|
Short videos Mowanjum Story What things can cause diabetes? Traditional tucker in town Dhalaleena's Story |
These short videos tell a story about some people with diabetes and how they improved their diabetes, about things that can cause diabetes, and about choosing traditional tucker. Developed by the Primary Care Nutrition Team TERHS, NT Health. |
Diabetes education opportunities for health professionals
| Resources | Description |
|---|---|
| Aboriginal and Torres Strait Islander Health - Diabetes e-Learning from the National Diabetes Services Scheme (NDSS) website. | Online learning modules for Aboriginal and Torres Strait Islander health workers and practitioners and health professionals working with Aboriginal and Torres Strait Islander Peoples living with diabetes. Developed by the NDSS. |
| National Diabetes Nursing Education Framework - Learning Modules from the National Diabetes Services Scheme (NDSS) website. | Online learning modules designed to help nurses gain foundation level knowledge in diabetes, but open to all health professionals wishing to improve knowledge in diabetes. Developed by the NDSS. |
| Webinar Series - Diabetes across the Lifecourse from the menzies school of health website. | A 10 part webinar series aimed at providing clinicians with comprehensive and up to date information to improve the care of Aboriginal and Torres Strait Islander young people with diabetes. Developed by Menzies School of Health Research. |
Website resources
- Australian Diabetes Educators Association (ADEA)
- Australian Diabetes Society (ADS)
- Australian National Diabetes Strategy 2021-2030
- Baker Heart and Diabetes Institute Central Australia
- Diabetes across the Lifecourse: Northern Australia Partnership - Menzies School of Health Research
- Diabetes Australia
- Diabetes Australia Position Statements
- Healthy Living NT
- Juvenile Diabetes Research Foundation
- National Diabetes Services Scheme (NDSS)
- National Obesity Strategy 2022–2032
- NT Primary Health Network – HealthPathways
Contact
Prevention and Wellbeing Unit
Strategy Planning and Reform
NT Health
Licensing and registration
Go to the Northern Territory Government website for more information on:
- accommodation and food businesses
- hairdressing, beauty therapy or body art
- liquor and hospitality
- farm management (including waste water)
- medical kits for remote areas authorisation
- medicines and poisons permits (including S4, S7 and S8 substances)
- medicines and poisons: retailers, wholesalers and manufacturers
- pest management technician licence (including fumigation endorsement)
- water licences/permits (including rainwater tanks).
Read more about:
Mental health information for health professionals
Nominations for Lived Experience Representatives
NT Health is calling for expressions of interest for two individuals with lived experience to provide a consumer, carer and/or community voice on the Mental Health Approved Procedures and Quality Assurance Committee.
By providing this consumer perspective, the lived experience representatives will help improve mental health and wellbeing outcomes for Territorians.
Successful applicants will be expected to attend up to four meetings per year, either face-to-face or via video conference and respond to requests for input or feedback on resources that are under development or review on an ongoing basis.
In you have any questions or wish to apply, please contact:
Mental Health Alcohol and Other Drugs Branch
Phone: 08 8999 2691
mhaod.doh@nt.gov.au
This information is for health professionals. For crisis counselling and other support areas please ring 1800 682 288 or go to the 24 Hour Mental Health Hotlines
The Mental Health Alcohol and Other Drugs Branch is a specialist policy and project unit within NT Health. It is responsible for:
- monitoring the delivery of mental health alcohol and other drugs services
- service development and integration
- mental health and alcohol and other drug legislative reform matters
- national mental health and alcohol and other drug reform agenda activities and projects
- provision of funding to non-government organisations.
Northern Territory Mental Health Clinical Collaborative
The Mental Health Clinical Collaborative brings together clinicians, service providers and community stakeholders to focus on the responsiveness and coordination of mental health care in the Northern Territory and the provision of timely and high quality appropriate care at the right place and at the right time.
Key functions
- To provide a mechanism for collaboration and communication between clinicians, service providers and community stakeholders.
- To promote an opportunity to exchange information, transfer knowledge, and discuss lessons learnt.
- To communicate alerts, directives and outputs or decisions relating to collaborations with national and international government and non-government agencies.
- To manage a program of service improvement initiatives, aligned with available resources.
Key principles
- Focus on the improvement in delivery of high quality mental health care and to improve the outcomes through a system wide approach.
- Support a patient-centred approach to care and service provision that meets individuals’ needs with emphasis on supporting and empowering people to achieve favourable healthcare experiences and outcomes.
- Engage with local health services to improve on current work and avoid duplication.
- Nurture the transformational changes in the health system to improve the clinical engagement with a focus on culture and leadership.
- Promote a culture of continuous improvement through informed best available evidence.
- Understand that the physical, social, spiritual and psychological approach to care requires consideration of a wider perspective.
- Be respectful in engagement with Aboriginal communities and respect the voices of Aboriginal individuals and communities.
Membership
Membership of the Mental Health Clinical Collaborative includes those who use and provide services across the continuum of care i.e. community members, academics/researchers and other representatives or class of representatives, as listed below:
- allied health practitioners
- Aboriginal health practitioners
- general practitioners (GPs)
- private practitioners
- the Aboriginal Medical Services Alliance Northern Territory (AMSANT)
- the Chief Health Officer
- the Chief Psychiatrist
- non-government organisations.
To join the Mental Health Clinical Collaborative:
Step 1. Fill in the expression of interest form.
Expression of interest form PDF (127.9 KB)
Expression of interest form DOCX (61.3 KB)
Step 2. Submit your form by mail or email:
Mental Health Alcohol and Other Drugs Branch
PO Box 40596
Casuarina NT 0811
mhaod.doh@nt.gov.au
Meeting dates
The Mental Health Clinical Collaborative meets 4 times per year.
Refer to the schedule for proposed meeting dates and times below.
| Date | Time | Venue | Room |
|---|---|---|---|
| Wednesday 4 May 2022 | 1:30pm to 3pm | Manunda Place, Darwin | DCVL2 Training Room |
| Wednesday 3 August 2022 | 1:30pm to 3pm | Manunda Place, Darwin | DCVL2 Training Room |
| Wednesday 2 November 2022 | 1:30pm to 3pm | Manunda Place, Darwin | DCVL2 Training Room |
| Wednesday 1 February 2023 | 1:30pm to 3pm | Manunda Place, Darwin | DCVL2 Training Room |
More information
For further information on the NT Mental Health Clinical Collaborative contact the Mental Health Alcohol and Other Drugs Branch by phone 08 8999 2691 or email mhaod.doh@nt.gov.au.
Protocol between NT Health and NT Police for mental health matters
The protocol for cooperative arrangements in mental health matters between NT Health and NT Police is an agreement between NT Police and NT Health to work in cooperation to promote a safe and coordinated system of response and care for people known, or suspected to be experiencing mental illness, disturbance or complex cognitive impairment, or exhibiting behaviours that may indicate such, and who may require care and treatment under the Mental Health and Related Services Act (MHARS Act) 1998.
Contact
Mental Health Alcohol and Other Drugs Branch - Darwin
PO Box 40596
Casuarina NT 0811
Phone: 08 8999 2691
mhaod.doh@nt.gov.au
For other related services, please contact:
- Northern Territory Mental Health Coalition (NTMHC) - peak body for community-managed mental health
- Community based mental health services - various non-government services
- NT Community Visitor Program - independent complaints, advocacy, monitoring and inspection body.
National Registration and Accreditation Scheme for health practitioners
Health practitioners in the NT are registered and regulated through the National Registration and Accreditation Scheme.
The Australian Health Practitioner Regulation Agency (AHPRA) was established to provide support to the National Boards.
Under the Health Practitioner Regulation National Law Act 2009, the Australian Health Ministers established national boards to regulate health professions in Australia:
Aboriginal and Torres Strait Islander Health Practice Board of Australia
Chinese Medicine Board of Australia
Chiropractic Board of Australia
Dental Board of Australia
Medical Board of Australia
Medical Radiation Practice Board of Australia
Nursing and Midwifery Board of Australia
Occupational Therapy Board of Australia
Optometry Board of Australia
Osteopathy Board of Australia
Paramedicine Board of Australia
Pharmacy Board of Australia
Physiotherapy Board of Australia
Podiatry Board of Australia
Psychology Board of Australia
Contact
Australian Health Practitioner Regulation Agency
Level 5
22 Harry Chan Avenue
Darwin NT 0800
Phone: 1300 419 495
Fax: (08) 8901 8502
www.ahpra.gov.au
Mail to
GPO Box 9958
Darwin NT 0801
National Critical Care and Trauma Response Centre
The National Critical Care and Trauma Response Centre (NCCTRC) is a key element in the Australian Government's disaster and emergency medical response to regional disasters.
The NCCTRC’s role is to make sure Royal Darwin Hospital can provide a rapid response in the event of a mass casualty incident in the region.
The centre has provided significant financial support to Royal Darwin Hospital to improve the ability of the hospital’s surgical and trauma divisions.
It also provides clinical and academic leadership in disaster and trauma care, as well as a local response capability and an international education, training and exercising capacity.
The NCCTRC is funded by the Australian Government through the Northern Territory Department of Health and was established following the 2002 Bali bombings.
Go to the National Critical Care and Trauma Response Centre website.
Northern Territory National Disability Insurance Scheme Restrictive Practices Authorisation
Northern Territory National Disability Insurance Scheme Restrictive Practices Authorisation
From 1 July 2019, all National Disability Insurance Scheme (NDIS) registered providers of disability supports in the Northern Territory (NT) must adhere to the NT National Disability Insurance Scheme (Authorisations) Act 2019 (the Act).
The Act works together with NDIS Quality and Safeguarding Framework and the NDIS Restrictive Practice and Behaviour Support Rules 2018 to ensure safeguards are in place for NDIS participants who may be vulnerable to the use of restrictive practices.
NDIS registered service providers who plan to implement a restrictive practice as part of an NDIS participant’s Behaviour Support Plan must submit a request for authorisation of a restrictive practice to the NT Senior Practitioner.
Authorisation of a restrictive practice is undertaken as part of a three stage process:
- The NDIS registered service provider requests for authorisation of a restrictive practice.
- The NT Senior Practitioner assessment of the authorisation request.
- Outcome of the NT Senior Practitioner decision.
The NT Restrictive Practice Authorisation Framework. PDF (669.8 KB) Guidelines for NDIS Service Providers provides details on the NT Restrictive Practice Authorisation process and related NDIS processes.
Request for authorisation of a restrictive practice
NDIS registered providers must complete an application for authorisation. To apply, all authorisation requests are to be submitted though the Restrictive Practice Authorisation System website.
All applications must include the following information:
- Particulars of the restrictive practice proposed to be applied to the participant.
- A copy of the NDIS Behaviour Support Plan (interim or comprehensive) that specifies the proposed restrictive practice.
- Consent of the NDIS participant to disclose information required for the application (RPA - 2A Disclosure Agreement by the NDIS Participant) - please note these documents must be attached to the online Apply for Authorisation link above.
- Evidence of consultation with the participant, their family, carers, guardian or other relevant person about the use of restricted practices as a component of their BSP (RPA - 2B Evidence of Consultation) - please note these documents must be attached to the online Apply for Authorisation link above.
- Particulars of the NDIS service providers who will apply the restrictive practice to the participant.
- A summary of every restrictive practices applied (both authorised and unauthorised) from the date of application and the preceding 12 months.
- Any other information the NDIS service provider considers relevant to the application, such as reportable incidents relevant to the application.
Applications for authorisation that do not meet the above mandatory information requirements; and which contain prohibited restrictive practices (the Act, Part3, S17) will not be accepted.
The NT Senior Practitioner assessment of the authorisation request
Assessment is undertaken by the NT Senior Practitioner in accordance with:
- the assessment criteria at section 4.2 (page 11) of the NT Restrictive Practice Authorisation Framework PDF (669.8 KB)
- the Guiding Principles of the Act (the Act, Part 1 Sec 5) and
- against the Behaviour Support Plan - Quality Evaluation II (BSP-QEII).
Outcome of the NT Senior Practitioner decision
The NT Senior Practitioner will provide an Assessment Outcome for action by the NDIS Service Provider, outcomes will be one of the following:
- Authorisation is provided. The NDIS provider can progress to the next stage.
- A request for further information and or recommendation for an alternative support.
- Authorisation not provided.
Unauthorised use of restrictive practices
Unauthorised use of restrictive practices in relation to an NDIS participant is a reportable incident as per the ‘NDIS (Incident Management and Reportable Incidents) Rules 2018’. NDIS information and processes for reporting an incident are at the NDIS website.
Any use of unauthorised restrictive practice(s) must be reported to the NDIS Quality and Safeguards Commission as a reportable incident until the behaviour support plan is “Activated” in the NDIS Commission portal. For further information go to the NDIS Quality and Safeguards Commission website.
Change in circumstances
If an NDIS Participant has a change in circumstances which results in no longer requiring involvement with the NT Restrictive Practices Authorisation Unit, the Service Provider must notify the Restrictive Practice Authorisation Unit via email as soon as practicably possible following the change in circumstance. Changes in circumstances may include, but are not limited to, an elimination of restrictive practice, interstate move, exiting the NDIS or notification of deceased participant.
Authorisations only apply to the jurisdiction they are made in
If an NDIS Participant with a restrictive practices in place moves to the Northern Territory from another jurisdiction, a new authorisation application will need to be made to the NT Restrictive Practices Authorisation Unit to ensure the restrictive practice meets the requirements of the Authorisation Framework.
Contact
All authorisation requests are to be submitted through the Restrictive Practice Authorisation System website.
Queries in regards to the NT NDIS Restrictive Practices Authorisation process can be emailed to the DoH Restrictive Practices Authorisation Unit at restrictive-practices.authorisation-unit@nt.gov.au.
Forms and Information
- Restrictive Practices Authorisation Unit Medication Purpose Form DOCX (696.2 KB)
- NT Restrictive Practices Authorisation Framework PDF (669.8 KB)
- NT Restrictive Practices Authorisation Framework - Plain Language PDF (780.1 KB)
- NT Restrictive Practices Authorisation Framework - Easy Read Guide PDF (5.2 MB)
- RPA - 2A Disclosure Agreement by the NDIS Participant DOCX (706.0 KB)
- RPA - 2B Evidence of Consultation Form DOCX (696.4 KB)
Nutrition and physical activity
NT Health seeks to improve the health and wellbeing of Territorians by supporting and developing a range of nutrition and physical activity health promotion initiatives including policy, supportive environments, health education and community action. Focus areas include overweight, obesity, reducing consumption of energy-dense, nutrient-poor food and beverages and encouraging active lifestyles.
Nutrition and physical activity policy statements
Evidence-based policy statements articulate the stance of NT Health on the following key topics:
Healthy choices made easy
The healthy choices made easy (HCME) policy regulates food and drink provision on NT Health premises ensure healthy options are always available.
Foods and drinks are grouped into green, amber or red categories based on their nutritional value. Green and amber foods and drinks should make up at least 80% of all foods and drinks provided or available for sale.
Read the full policy:
See publications below for more information about food and drinks provision policy in NT Health facilities.
Publications
| Title / description | Location |
|---|---|
| Ideas for feeding. These fact sheets have ideas for feeding infants, children and fussy eaters. | |
| Australian dietary guidelines | Go to the Eat for Health website |
| Australia’s physical activity and sedentary behaviour guidelines | Go to the Department of Health website |
Healthy Living for Children and Teenagers Above a Healthy Weight A child nutrition client education resource designed for use with children who are above a healthy weight (aged 5-18 years) and their families. Health Professionals Guide: | Healthy Living for Children and Teenagers Above a Healthy Weight |
Feeding Babies Resource for remote communities. This information is about feeding babies from birth to early childhood. | Feeding Babies |
Growing Healthy Kids (2019) Designed for use with families with young children who are growth faltering or are at risk of growth faltering | Growing Healthy Kids |
Good Food for Strong Blood Designed for use with families with young children who have iron deficiency anaemia (weak blood) | Good Food for Strong Blood |
Good Food for Diabetes Resource for remote communities. | Good Food for Diabetes |
Healthy Choices Made Easy: NT Health Food and Drinks Provision | Healthy choices made easy policy Frequently asked questions |
| School Nutrition and Healthy Eating policy, guidelines and supporting documents | School nutrition and healthy eating policy |
Nutrition Education Resource Manual (NERM) The NERM is a compilation of activities and resources developed to support the introduction of nutrition education and healthy eating habits to primary aged students. | Nutrition Education Resource Manual |
Long Day Care Menu Planner This planning tool can assist long day care providers to review their menus and determine whether nutritional requirements of their children are being met. | Long day care menu planner |
|
Let’s get Going! (2022) How to start a parent-led exercise group for children 1-5 years | Let’s get Going! (2022) |
Let’s Dig! A school garden resource This teachers’ resource offers ideas and activities to run four components of a School Garden unit of work. Suitable for Transition through to Year 6 students. | Let's Dig! A School Garden Resource |
Live Lighter Live Lighter supports professionals in the health, workplace and community sector to help their clients to eat well and move more. | Live Lighter for Professionals |
The Flour Drum Stove Cookbook This book shows how to make and cook on a flour-drum stove, and includes recipes suitable for families in remote areas. | The Flour Drum Stove Cookbook |
Kukumbat Gudwan Daga: Really Cooking Good Food Healthy cookbook for feeding ten or more people. | Kukumbat gudwan daga: really cooking good food |
Market Basket Survey Reports An annual survey monitoring food cost, availability, variety and quality in remote community stores. | Market Basket Survey Reports |
| Remote Stores Newsletter Archive 2013 - 2018 | Remote Stores Newsletter |
Remote Indigenous Stores and Takeaways (RIST) The RIST resource range largely remains relevant to establish and improve standards for healthy remote stores. It includes guidelines, checklists and strategies for improving access to a healthy food supply and standards in remote stores. | Remote Indigenous Stores and Takeaways Project |
Healthy Stores 2020 - Policy Action series Evidence-based policy action series for effective health-promoting merchandising techniques in remote community stores, by RE-FRESH Centre of Research Excellence | Actions for Healthy Stores in remote Aboriginal and Torres Strait Islander Communities in Australia |
More information
For more information contact:
Health Improvement
GPO Box 40596
Casuarina NT 0811
healthpromotionnt@nt.gov.au
Ophthalmology
NT Health offers two public ophthalmology services across the Northern Territory:
- Alice Springs Hospital Ophthalmology Department that services Central Australia and Barkly regions
- Royal Darwin and Palmerston Hospital that services the Darwin, Big Rivers & East Arnhem regions.
Both services deliver a wide range of clinical and surgical services across the whole NT, including patients from eastern Western Australia and northern South Australia.
Referral guidelines
All referring health professionals should adhere to the below guidelines:
Outreach program
Ophthalmology Outreach services are federally funded by these NT Health programs to deliver services across all NT regional hospitals and remote communities:
- Rural Health Outreach Fund
- NT Primary Health Network, Medical Outreach Indigenous Chronic Disease.
The programs are modelled to include regular scheduled visits to the main regional hospitals (Tennant Creek Hospital, Katherine Hospital and Gove District Hospital) to enable regular monitoring and treatment, including intravitreal injections, glaucoma management and timely cataract surgery for our patients in those regions.
The teams visit remote communities across the NT, which are screened by the Visiting Optometrist Scheme (VOS). It is generally preferred that initial screening is first performed by the optometrist through VOS to assist triaging and avoid delays in management. This allows patients, who need specialists care, to be seen where most appropriate.
Majority of ophthalmology patients require comprehensive testing from various machines, which are not available in the remote communities. To avoid duplicate patient episodes it is preferable to refer patients directly to the regional service.
Go to our public visit calendar.
Visiting Optometrist Scheme (VOS)
VOS is a federally funded program which aims to increase optometric services to regional and remote locations. The optometrists provide primary eye care services for remote NT patients and coordinate ongoing care plans with ophthalmology. Their services include:
- general eye care screening
- diabetes eye checks
- spectacle prescription
- post-operative cataract/pterygium follow up.
To find out which provider services a particular community, email VOS.DoH@nt.gov.au
Driving requirements
Read the below information before assessing NT driving requirements:
- Medical fitness to drive on the Northern Territory Government website
- Visual acuity for current driving requirements on the Austroads website.
Student placements
Orthoptic students
The ophthalmology departments offer student placements to orthoptic students. Placements in the NT expose students to a range of learning, and may include the opportunity to participate in our Outreach program. For more information email:
- Royal Darwin and Palmerston Hospital: Orthoptist.TEHS@nt.gov.au
- Alice Springs Hospital: eyebookingofficerash.doh@nt.gov.au
Medical students
Flinders University allocates placements to medical students. Placements in the NT expose students to a range of learning, and may include the opportunity to participate in our Outreach program. For more information email:
- Flinders NT Placements: fnt.placements@flinders.edu.au
Oral health information for health professionals and schools
Fluoride varnish program in remote schools
The School Based Fluoride Varnish Program (SBFVP) is available for implementation in Top End remote schools. The program opens pathways to important early intervention dental treatment for Top End children.
The program aims to improve oral health and increase dental hygiene awareness across school communities, and:
- Slow or stop the progress of dental decay
- Detect disease in high-risk children and open pathways to treatment
- Provide early intervention, reducing emergency dental appointments and prevent hospitalisation
- Provide a welcoming orientation to the dental clinic
- Increase oral hygiene awareness in the community.
In the below video Dental Therapist, Jo Bremner and Moulden Park School Principal, Ali Brady share insights about the School Based Fluoride Varnish Program and the success they have seen since the program commenced in November 2018.
Enrol your school in the program
Schools in remote regions can express their interest in participating in the program by contacting oralhealth.THS@nt.gov.au
Participating schools are required to:
- issue SBFVP consent forms to all existing school students (these remain current from preschool to grade 6)
- include SBFVP consent form in the new enrolment pack for any new students or any students commencing in the next year
- send copies of all consents forms to: oralhealth.THS@nt.gov.au with “SBFVP” in the subject line
- provide updated class lists to Top End Oral Health team prior to each visit
- plan dates at six monthly intervals for four visits.
The Top End Oral Health team will:
- collate consent forms
- enter all children in their class groups into the Titanium client database
- check when/if child has had Fluoride Varnish applied
- review medical history.
Treatment process
The Top End Oral Health team will attend the school and negotiate the most suitable method of moving children from their classrooms to the Fluoride Varnish treatment area, and back again.
The program averages 50 children per day so a school population of 250 will take five days.
If a child is unable to cope with dental treatment at the dental clinic, they will be referred to the hospital to have the treatment carried out under general anaesthetic.
About fluoride varnish
Plaque bacteria in the mouth react with sugar to form acids, which strip minerals from the tooth structure. This damage to the tooth is referred to as tooth decay. Tooth decay, if left untreated, will progress, leading to the loss of the tooth.
The application of Fluoride Varnish is recognised as a safe and effective way for slowing and reducing decay and to assist in preventing new cavities. Professionally applied Fluoride Varnish contains fluoride ions suspended in an alcohol and resin base.
Fluoride Varnish sets immediately on contact with saliva and forms a waxy film, which adheres to teeth. This is gradually worn off by chewing or brushing. Fluoride Varnish is well tolerated by children, and is relatively easy to apply.
The recommended frequency of application of fluoride varnish is twice per year, however for individuals at higher risk of dental caries and/or without access to a fluoridated water supply, more frequent applications may be recommended.
While highly effective, Fluoride Varnish is not regarded a replacement for a child’s regular check-ups. Regular dental check-ups are vital for all children.
- The regular application of Fluoride Varnish will repair early damage.
- The earlier a tooth is treated the less invasive the dental experience.
- Children who do have tooth decay may require treatment under general anaesthetic.
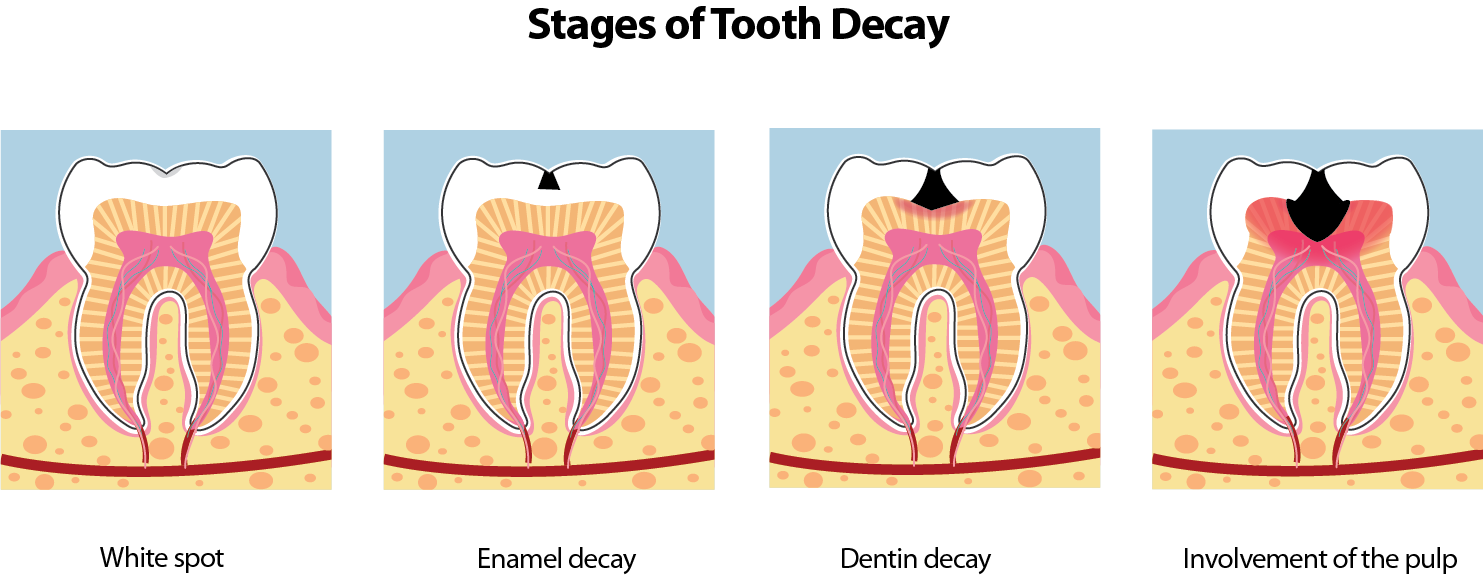
- White spot stage
The regular application of Fluoride Varnish at this stage (early intervention) will replenish the lost minerals and repair the damage.
- Enamel and dentine decay
At this stage the tooth will not be painful but does requires clinical treatment. The earlier this damage is identified and treated (early intervention) the less invasive the treatment is and the tooth will be saved.
- Involvement of the pulp
When tooth decay is left untreated and affects the pulp, toothache occurs. In baby teeth this will necessitate an extraction. Extraction of baby teeth can lead to orthodontic problems in the future. It is also a distressing process for the child and family.
Fluoride Varnish Program background
The program was trialled at Moulden Park Primary School in November 2018. Following its successful implementation, it then commenced in 2019 in eight schools in Darwin, Nhulunbuy and Katherine.
Territory children, particularly those from disadvantaged groups, have some of the worst oral health outcomes in Australia. Data from the most recent National Child Oral Health Study found Territory children were more likely to have tooth decay and this was likely to be of greater severity than children elsewhere in the country.
The uptake of child dental services by disadvantaged groups is low and the oral disease burden high. Disadvantaged groups include:
- children from low socio-economic areas
- Aboriginal people.
Contact us
For further information please contact: oralhealth.THS@nt.gov.au
Patient travel: health professionals
The Travel Management System (TMS) is the online system used by the Department of Health to log all requests from the Patient Assistance Travel Scheme (PATS) including:
- Inter Hospital Transfers (IHT)
- medical retrieval services
- intra and interstate travel
Read about the Patient Assistance Travel Scheme (PATS).
Login
Login to TMS here
Who can use TMS
TMS is for Department of Health staff and external health providers including:
- remote community clinics
- GPs and private medical practices.
TMS approval
To access TMS submit an application form to tms.ths@nt.gov.au.
The system automatically approves basic travel requests, all other requests are processed as follows:
Step 1. Requests for intra and interstate travel, Inter Hospital Transfers and medical retrieval are sent to a delegate officer for approval.
Step 2. The requesting doctor or clinic is emailed the outcome of the request. If the travel is denied, the reason will be provided.
Step 3. PATS office staff book approved travel requests, unless the patient chooses to book their own and claim reimbursement.
Step 4. The requesting doctor or clinic will receive an itinerary to give to the patient.
Training
TMS training is delivered in person, over the phone or online through GoToMeeting training sessions.
Training manuals and video tutorials are available on TMS under the 'get assistance' tab.
Privacy
No medical information is included in emails from the TMS system to the person approving travel. It is only accessible from the secure TMS site.
All Department of Health users are bound by the Information Privacy Principles under the Northern Territory Information Act.
All external users are bound by the Privacy Principles under the Privacy Act. Read the Act on the Office of the Australian Information Commissioner website.
All health professionals using the TMS are also bound by the relevant Registered Health Professionals Code of Ethics.
Contact
For general enquiries or to book a TMS training session email tms.ths@nt.gov.au or call (08) 8999 2514.
Public health licensing and regulation
For information about registering public health premises, go to the Northern Territory Government website:
For information about public health regulations, view environmental health contacts.
Remote Health Atlas
This site provides remote health resources for non-government health services and agencies.
- Clinical Protocols
- Emergency Kits
- Evacuation Centre Management
- Health Record Guidelines
- Health Record Application Forms
- Medical Students
- Men’s Business
- Pathology Stores Order Forms
- Pharmacy Guidelines
- Pharmacy Forms
- Pharmacy Resources
- Point of Care Pathology
- Research Proposals
- Specialist and Clinical Services Outreach
Contact:
For further information e-mail: CAProfPracNurse.THS@nt.gov.au
Rural Generalist Pathway
“A Rural Generalist is a medical practitioner who is trained to meet the specific current and future healthcare needs of Australian rural and remote communities, in a sustainable and cost-effective way by providing both comprehensive general practice and emergency care and required components of other medical specialist care in hospital and community settings as part of a rural healthcare team.”
Collingrove Agreement.
NT Health is committed to supporting professionals who choose the Medical Rural Generalist Pathway and is experienced in facilitating the transition for rural generalist trainees through the various educational and training components for the first six years of post-graduate training.
The training pathway supports medical officers with targeted training and development to become a Rural Generalist. It is a selective and flexible pathway that offers medical officers the opportunity to explore a wide variety of clinical training and develop the advanced skill set required to support the health needs of rural communities.
The Rural Generalist Coordination Unit is working with local and national stakeholders to strengthen existing pathways and incorporate them into a well-structured Rural Generalist Pathway aligned to the national strategy.
The collaboration of key stakeholders has an objective to get more doctors into rural and remote areas, and to better equip these doctors to meet community needs.
Resources
These pages have information about training, education and employment opportunities for current and future health professionals:
For more information about student placements, work experience and Indigenous cadetships with NT Health go to:
Publications
- Stronger Rural Health Strategy
- Policies/guideline – to be developed
- Strategies – to be developed
Contact
Rural Generalist Coordination Unit
rural.generalist@nt.gov.au
Phone: 08 8924 4150
Web: Rural Generalist
Sepsis information and resources
The NT Health sepsis pathways are for use in all settings. They incorporate evidence-based risk criteria to help clinicians recognise sepsis early and support early escalation of care and management.
NT Health sepsis pathways can be ordered via Darwin (HR number) or Alice Springs (HPS code) Stores. Follow local processes for ordering for your specific work area.
| HPS code | HR number | Sample | Pack quantity |
|---|---|---|---|
| HR543-02/23 | Acute care adult sepsis pathway - Top End, East Arnhem and Big Rivers regions PDF (376.2 KB) | ||
| HR543a-02/23 | Acute care paediatric sepsis pathway - Top End, East Arnhem and Big Rivers regions PDF (300.4 KB) | ||
| 174905 | HR543b-02/23 | Primary health care adult sepsis pathway PDF (180.6 KB) |
Pack = 50 forms (replenishment and purchase unit) |
| 174906 | HR543c-02/23 | Primary health care paediatric sepsis pathway PDF (178.4 KB) |
Pack = 50 forms (replenishment and purchase unit) |
| 174907 | HR543d-02/23 | Acute care adult sepsis pathway - Central Australia and Barkly regions PDF (372.4 KB) |
Pack = 50 forms (replenishment and purchase unit) |
| 174908 | HR543e-02/23 | Acute care paediatric sepsis pathway - Central Australia and Barkly regions PDF (299.4 KB) |
Pack = 50 forms (replenishment and purchase unit) |
Guidelines
The NT Health sepsis guidelines are intended to support the sepsis pathways and provide further guidance in:
- Best practice and a consistent approach across all NT health services for early sepsis recognition and management.
- Where sepsis is suspected, empower staff to escalate care to clinicians experienced in recognising and managing sepsis.
- Engaging senior medical staff in sepsis recognition and management of patients.
- Supporting the provision of education and information for patient and carers.
For acute care:
- Adult acute care - NT Health sepsis recognition and management guideline PDF (1.4 MB)
- Paediatric acute care - NT Health sepsis recognition and management guideline PDF (1.1 MB)
For primary health care:
- Adult primary health care - NT Health sepsis recognition and management guideline PDF (1.1 MB)
- Paediatric primary health care - NT Health sepsis recognition and management guideline PDF (1021.0 KB)
The Remote Health Atlas or Primary Health Network sites have updated their sepsis guidelines to align with NT Health to ensure consistency of practice across the NT.
Sepsis clinical care standard
The goal of the sepsis clinical care standard is to ensure that a patient presenting with signs and symptoms of sepsis receives optimal care, from symptom onset through to discharge from hospital and survivorship care.
This includes timely recognition of sepsis, early and appropriate antimicrobial therapy and continuity of care from the acute setting through to discharge and survivorship (Australian Commission on Safety and Quality in Health Care (ACSQHC), 2022).
The sepsis clinical care standard is linked to the antimicrobial stewardship clinical care standard, for more information go to the ACQHC website.
Online learning modules
A sepsis e-learning module, Sepsis Introduction, is available to all health professionals via MyLearning. This module helps clinicians to understand what sepsis is, its impact in the NT, how to identify and manage sepsis, and with the use of case studies, assists in applying the sepsis pathways into practice.
A sepsis e-learning module is available from the Remote Area Health Corps (RAHC) e-learning site. This is for all health professionals who want to learn more about sepsis. The e-module uses case studies to familiarise you with the NT Health sepsis pathways and tests your knowledge about sepsis recognition and management processes.
To complete the learning module, go to the RAHC website.
National sepsis resources
World Sepsis Day toolkit
Help to spread awareness about sepsis and World Sepsis Day in your workplace with free access to resources and fun activities.
Read more about World Sepsis Day Toolkit
The Pocketbook of Sepsis
A comprehensive digital library of evidence-based lectures presented by renowned international experts, brought to you by Sepsis Australia, and Continulus, a socially responsible healthcare learning platform. The ultimate goal is to make expert knowledge easily accessible to healthcare professionals worldwide, including those practicing in resource-limited settings.
Read more about The Pocketbook of Sepsis.
Continulus Library
Find a suite of free sepsis resources, including free CPD/CME-accredited lectures from some of the leading sepsis experts in the world.
Read more about Continulus Library.
2023 World Sepsis Congress
On April 25 and 26, 2023, the 4th World Sepsis Congress took place. Over the course of two days and 16 highly relevant and diverse sessions, more than 85 speakers from more than 35 countries presented on all aspects of sepsis, including the link to pandemics and AMR, the role of AI, ML, big data, patient safety, the impact of policy, novel trial design, the latest research, and much more.
Resources for the clinical nurse educator
Watch the sepsis pathophysiology video.
World Sepsis Day quiz cards - host your own game show
Download the World Sepsis Day quiz cards PUB (186.0 KB).
Resources for the medical officers
Septris 2.0 is a mobile-accessible, case-based, online game launched worldwide and developed for hospital-based medical and surgical, intensive care and emergency department physicians and nurses for treating Sepsis.
Read more about Septris 2.0

Information for health professionals
Adult patients
| Type | Resource | Website |
|---|---|---|
| Document | Epidemiology of Sepsis in Australian Public Hospitals | ACSQHC |
| Journal | The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3) | JAMA Network |
| Journal | Sepsis in the tropical Top End of Australia’s Northern Territory: disease burden and impact on Indigenous Australians | Medical Journal of Australia |
| Website | Surviving Sepsis Campaign Guidelines 2021 | Society of Critical Care Medicine |
| Document | Review of trigger tools to support the early identification of sepsis in healthcare settings | ACSQHC |
| Journal | Sepsis - Pathophysiology and Therapeutic Concepts | Frontiers |
| Document | Stopping Sepsis: A National Action Plan | George Institute |
| Document | Diagnosis and management of sepsis in the older adult | BMJ Publishing Group Ltd |
Rosie’s Story (3:16)
Surgical site infection leads to sepsis.
Ann’s Story (3:57)
Cancer survivor – post port-a-cath insertion infection that leads to death.
Geoff’s Story (8:13)
Splinter leads to septic shock.
Fiona’s Story (1:47)
Bump on elbow leads to sepsis.
Paediatric patients
| Type | Resource | Website |
|---|---|---|
| Document | Surviving sepsis campaign international guidelines for the management of septic shock and sepsis-associated organ dysfunction in children | Australian Sepsis Network |
| Website | Sepsis in children | BMJ Best Practice |
| Website | Children - Sepsis Alliance | Sepsis Alliance |
| Website | The current and future state of pediatric sepsis definitions: An international survey | American Academy of Pediatrics |
| Website | Sepsis prediction in hospitalized children: Model development and validation | American Academy of Pediatrics |
| Website | Sepsis prediction in hospitalized children: Clinical decision support design and deployment | American Academy of Pediatrics |
| Document | International Consensus Criteria for Pediatric Sepsis and Septic Shock PDF (793.6 KB) | American Medical Association |
| Website | Australia's Silent Killer | 7 News Facebook |
Mia’s Story (3:18)
Pre-hospital symptoms, if you are worried get help/go to ED.
Beauden’s Story (13:11)
From scrape to knee to septic shock, includes survivorship care/follow up.
Sepsis and Children (13:28)
From infected cut to quadruple amputation – includes globally recognised leading expert on sepsis in children.
Australian Story – Mia’s Story (8:06)
Sunrise article – family shares Mia’s story of surviving sepsis.
Neonatal
| Type | Resource | Author |
|---|---|---|
| Journal | Diagnosis of neonatal sepsis: The past, present and future | International Pediatric Research Foundation, Inc |
| Journal | Diagnosis of neonatal sepsis: The role of inflammatory markers | Medical University of Graz |
| Journal | Neonatal sepsis definitions from randomised clinical trials | European Society for Paediatric Research (ESPR) |
| Website | Sepsis Australia | Australian Sepsis Network |
| Website | The George Institute for Global Health | The George Institute for Global Health |
| Website | Australian Commission on Safety and Quality in Health Care | Australian Commission on Safety and Quality in Health Care |
Global Health – Newborn Care Series (5:51)
Shows baby with sepsis, how to evaluate and treat.
Neonatal Sepsis: Newborn Blood Infection (4:37)
Causes, symptoms and treatment by Dr Nanditha, Neonatologist at Kangaroo Care.
Isla’s Story (3:42)
Baby wakes up lethargic, emergency transfer to Perth Children’s Hospital, signs and symptoms.
Maternity
| Type | Resource | Website |
|---|---|---|
| Website | Pregnancy and childbirth | Sepsis Alliance |
| Journal | Azithromycin to prevent sepsis or death in women planning a vaginal birth | A-PLUS Trial Group |
Maile’s Story – Maternal Sepsis (7:32)
Mother develops sepsis after returning home post birth.
Kayleigh’s Story (6:39)
Mother develops sepsis at 7 months gestation leading to quadruple amputation.
Amanda’s Story (6:04)
Mother develops sepsis 6 weeks post a traumatic birth.
For all patient cohorts
Public awareness information
Campaign resources
| Type | Resource | Author |
|---|---|---|
| Poster | NT Health developed in partnership with ACSQHC | |
| Brochure | NT Health developed in partnership with ACSQHC |
Spotlight on sepsis (1:55)
NT Health developed in partnership with ACSQHC.
Signs and Symptoms (0:52)
NT Health developed in partnership with ACSQHC.
National websites
| Type | Resource | Website |
|---|---|---|
| Website | What is sepsis? | Global Sepsis Alliance |
| Website | Life after sepsis: A guide for survivors, carers and bereaved families | Australian Sepsis Network |
| Website | National Sepsis Program | Australian Commission on Safety and Quality in Health Care |
Support groups
| Type | Resource | Author |
|---|---|---|
| Website | Australia and NZ Sepsis Support Group Facebook page | Australia and NZ Sepsis Support Group |
| Website | Patients and family | Sepsis Alliance |
| Website | Is it sepsis? | T for Thomas |
Contacts
For more information and assistance, contact Clinical Excellence and Patient Safety by emailing SafetyandQuality.DoH@nt.gov.au.
Sexual health
To contact NT Heath’s policy and strategy development unit, email Sexual Health and Blood Borne Viruses on SexualHealthandBloodBorneViruses.PublicHealthDirectorate@nt.gov.au
To contact Clinic 34, the NT Health’s regional health services delivering sexual health services, go to the Northern Territory Government website.
Shared models of care
This information is for health professionals. For information to the general public, go to the pregnancy screening and testing page.
The below document provides guidance for general practitioners participating in shared models of care across the Darwin and Palmerston regions in the schedule of care at antenatal visits for pregnant women.
Specialist Outreach NT (SONT)
Specialist outreach services in the Northern Territory (SONT) provide the logistics and coordination to support remote health visits. SONT is also a liaison point between remote clinics and specialists.
Clinical specialist services are accessed through:
- outreach to remote-living patients
- outpatient care delivered from hospitals
- TeleHealth consultations.
Find out what types of services are available in remote communities and how to meet with a visiting medical service.
Funding
In addition to major funding from the Northern Territory Government, SONT is assisted by the Australian Government's Rural Health Outreach Fund (RHOF - formerly known as MSOAP).
This provides important support to the travel and administrative expenses of outreach service delivery.
Contact
SONT Operations Manager
Phone: (08) 8999 2518
SONT.DHF@nt.gov.au
Territory Equipment Program (TEP) and the Seating Equipment and Technical Service (SEAT)
This page includes information for health professionals, guidelines, forms, policies and procedures for the Territory Equipment Program (TEP) and the Seating Equipment and Technical service (SEAT).
Territory equipment program (TEP)
The Territory Equipment Program, provides community equipment and aids to children and adults who live in the community and have a functional impairment that requires prescribed equipment, aids and appliances that assist in maintaining and improving their capacity to live and participate in everyday activities.
TEP approved prescribers
- AP-1 TEP Professional Criteria for Approved Prescribers DOCX (79.7 KB)
- AP-2 TEP Application for App Prescriber Registration DOCX (70.0 KB)
TEP clinical guidelines
- CG-1 Communication Aids and Devices DOCX (81.0 KB)
- CG-2a ADLs Toileting Aids DOCX (78.1 KB)
- CG-2b ADLs Showering Aids DOCX (77.8 KB)
- CG-2c ADLs Transfer Aids and Lifting Devices DOCX (75.7 KB)
- CG-2d ADLs Miscellaneous Items DOCX (76.2 KB)
- CG-3 Bed Equipment DOCX (80.8 KB)
- CG-4 Pressure Management Equipment DOCX (81.5 KB)
- CG-5 Wheeled Mobility Aids DOCX (85.4 KB)
- CG-6 Ambulant Mobility Aids DOCX (75.9 KB)
- CG-7 Home Modifications DOCX (83.0 KB)
- CG-8 Personal Emergency Response System DOCX (80.3 KB)
- CG-11 Oxygen DOCX (64.6 KB)
- CG-12 Continence Aids DOCX (77.9 KB)
TEP fact sheets
- AE - TEP Alternate Equipment Sources DOCX (58.7 KB)
- FS-2 TEP Repair and Maintenance Fact Sheet DOCX (86.1 KB)
- FS-2 TEP Repair and Maintenance Fact Sheet (Easy Read) DOCX (56.9 KB)
- FS-1 TEP Fact Sheet DOCX (57.1 KB)
- FS-P TEP Moving Interstate Aids and Equipment Fact Sheet DOCX (57.9 KB)
TEP forms and agreements
- A1 TEP Application Form DOCX (72.5 KB)
- A1-E TEP Application for special consideration DOCX (53.9 KB)
- EA-O TEP Optometry Assessment DOCX (55.1 KB)
- EA-D TEP Driving assessment for powered mobility aids DOCX (56.0 KB)
- FC-1 TEP Flowchart DOCX (82.6 KB)
- FC-2 TEP Eligibility Flowchart DOCX (88.2 KB)
- GL-TEP Glossary DOCX (63.9 KB)
- GR-C TEP Grab Rail Owner Landlord Consent DOCX (52.4 KB)
- GR-D TEP Grab Rail Disclaimer Form DOCX (50.6 KB)
- HD Home Modification Diagram DOCX (55.4 KB)
- HM-1 TEP Home Modifications Agreement Owners and DEP with deed DOCX (48.7 KB)
- HM-1A TEP Home Modifications Agreement Owners and Builder Schedule A DOCX (49.2 KB)
- HM-C TEP Home Modifications Certificate of Completion DOCX (48.7 KB)
- HM-D TEP Home Modifications Disclaimer Form DOCX (50.9 KB)
- O2 Oxygen Delivery/Collection Request DOCX (55.2 KB)
- OW-1 Transfer Ownership to TEP DOCX (55.5 KB)
- OW-2 DEP Transfer Ownership from TEP DOCX (55.7 KB)
- SF-1 TEP Satisfaction form DOCX (67.2 KB)
- SL-1 Equipment Register Template DOCX (48.2 KB)
- SL-2 Returned Equipment Advice DOCX (54.8 KB)
- SL-3 TEP Hold Equipment Advice DOCX (59.4 KB)
- T1 TEP Trial Request DOCX (52.0 KB)
- T2 Agreement to Trial TEP Equipment DOCX (51.1 KB)
- T3 TEP Trial Log for Powered Mobility Aids DOCX (59.1 KB)
TEP policies
- PO-1 TEP Policy DOCX (93.8 KB)
- PO-2 TEP Financial Eligibility Policy DOCX (90.2 KB)
- PO-3 TEP Access to Services Policy DOCX (92.8 KB)
- PO-4 TEP Prioritisation Policy DOCX (88.5 KB)
- PO-5 TEP Client Contribution Policy DOCX (92.3 KB)
- PO-6 TEP Ownership and Portability Policy DOCX (92.5 KB)
- PO-7 TEP Management of Equipment Policy DOCX (91.5 KB)
- TEP Approved Equipment List DOCX (93.1 KB)
TEP prescription forms
- P-0 Prescription Form for Multiple Level 1 DOCX (71.0 KB)
- P-1 Communication Aids and Devices DOCX (68.2 KB)
- P-2 Aid for Daily Living DOCX (68.6 KB)
- P-3 Bed Equipment DOCX (73.2 KB)
- P-4 Pressure Management Equipment DOCX (76.3 KB)
- P-5 Wheeled Mobility Aids DOCX (73.5 KB)
- P-7 Home modifications DOCX (62.3 KB)
- P-8 Personal Emergency Response System DOCX (74.8 KB)
- P-9 Continence aids DOCX (69.5 KB)
- P-11 Oxygen DOCX (66.0 KB)
Seating equipment and technical service (SEAT)
The Seating equipment and technical service (SEAT) is a Northern Territory Government service that provides customised pressure care, mobility, and seating equipment to children and adults who have a functional impairment with intermediate to complex seating, wheeled mobility, pressure care and assistive technology needs. SEAT Service provides necessary modifications to prescribed wheelchairs as well as fabrication of customised seating systems and pressure cushions.
The SEAT service provides clinical consultancy and technical services and will individually assess each client referred to them, in consultation with the treating therapist and or carer/family member to ensure the prescription is the most suitable.
Therapists can contact SEAT at any time for advice on customisations and modifications to seating and wheelchairs. Training and SEAT Service clinics are provided in urban and remote locations throughout the Northern Territory.
SEAT Contacts
Top End
Phone: (08) 89228228
Email: SEATDarwin.THS@nt.gov.au
Central Australia
Phone: (08) 89516744
Email: centralaustraliaintake.THS@nt.gov.au
Women's health information for professionals
The Women’s Health Strategy Unit develops and supports population services and programs that improve health outcomes for women in Northern Territory (NT).
The core business of the Women’s Health Strategy Unit is to provide the following:
- policy development
- program development
- health promotion
- population health program advocacy.
Role
The role of the Women’s Health Strategy Unit is to:
- identify the issues and needs affecting women in the NT, as well as the determinants of these issues
- define and develop population health strategies (based on the best available evidence) to address the issues and needs and support their placement in HHS agreements
- ensure that funding agencies are informed about the health and developmental needs of women in the NT
- support implementation of the selected strategies by NT service agencies
- measure, analyse and evaluate the impact in the NT of implemented strategies
- participate (or lead) national and jurisdictional development of policies and programs aimed at improving women’s health, including access to services.
The following principles underpin the work of the unit:
- importance of a systems-based approach
- commitment to program efficacy and evidence-based practice
- valuing partnerships
- supporting community engagement
- respect for Aboriginal cultural security
Projects
The unit is committed to the following projects and strategic plans:
- leading the implementation of the NT Government’s Domestic and Family Violence Reduction Strategy, Safety is Everyone’s Right, across NT Health
- developing a transgender policy and associated resources for NT Health
- updating the child and adult sexual assault guidelines and development of NT Health policy
- providing policy advice in relation to NT abortion law reform.
Termination of pregnancy law reform
The Discussion Paper, Termination of Pregnancy Law Reform; Improving access by Northern Territory women to safe termination of pregnancy services, was released by the Department of Health on 9 December 2016 and submissions closed on the 27 January 2017.
Below is a summary of the key issues arising from consultations on the Discussion Paper.
Below are submissions the department received, with consent to publish:
Termination of Pregnancy Law Reform Bill
The Termination of Pregnancy Law Reform Bill was passed on 21 March 2017. It will commence on 1 July 2017.
Publications
Contact
Women’s Health Strategy Unit
GPO Box 40596
Casuarina NT 0811
Phone: (08) 8985 8018
Internal mail
Floor 4, Darwin Plaza
Smith Street
Darwin NT 0800
Telehealth for NGOs and other health professionals
This page is for non-government organisations (NGOs) or other health professionals.
Telehealth is real-time remote consultation using audio-visual information and communication technology, including phone or video appointments.
If you are a patient, go to the Northern Territory Government website.
Who to contact
You should call the contact details provided on your appointment letter for:
- technical problems
- re-scheduling of your appointment.
Specialist clinic contact details
Royal Darwin Hospital
Phone: 08 8922 8888
nt.gov.au/wellbeing/hospitals-health-services/royal-darwin-hospital
Palmerston Regional Hospital
Phone: 08 7979 9704
nt.gov.au/wellbeing/hospitals-health-services/palmerston-regional-hospital
Alice Springs Hospital
Phone: 08 8962 4399
nt.gov.au/wellbeing/hospitals-health-services/alice-springs-hospital/contact-alice-springs-hospital
Katherine Hospital
Phone: 08 8973 9211
nt.gov.au/wellbeing/hospitals-health-services/katherine-hospital
Tennant Creek Hospital
Phone: 08 8962 4399
nt.gov.au/wellbeing/hospitals-health-services/tennant-creek-hospital
Gove District Hospital
Phone: 08 8987 0211
nt.gov.au/wellbeing/hospitals-health-services/gove-district-hospital
Virtual waiting areas
If you have a telehealth appointment with NT Health, select the correct Healthdirect Video Call waiting area link below to access your appointment.
Top End
- Centre for National Resilience (CNR)
- COVID of Concern HITH
- Mycobacterium Clinic CDC Darwin
- NT BreastScreen
- DLNT
- NT Genetics
- NT Health Teletrials Clinic
- NT Health Test Clinic (for training only)
- PRH Rehabilitation
- RDH Allergy
- RDH ALO/Interpreter
- RDH Cardiology
- RDH Dermatology
- RDPH Diabetes/Endocrinology
- RDH Ear Nose & Throat (ENT)
- RDH Gastroenterology
- RDH General Medicine
- RDH General Surgery
- RDH Haematology
- RDH Hand & Plastics
- RDH Hepatology
- RDH Infectious Diseases
- RDH Intensive Care (ICU)
- RDH Maxillofacial
- RDH Medical Oncology Clinic (MOC)
- RDH MFM Telehealth
- RDH Neurology
- RDH Neurosurgery
- RDH Ophthalmology
- RDH Orthopaedic
- RDH Palliative Care
- RDH Preadmission Telehealth
- RDH Radiation Oncology Clinic
- RDH Renal
- RDH Respiratory & Sleep Services
- RDH Rheumatology
- RDH Surgical Scope
- RDH Urology
- RDH Vascular
- RDPH Allied Health
- RDPH@Home
- RDPH Viral Hepatitis
- RDH Women, Children and Youth Outpatients
- TE AOD Access Team
- TE AOD Inpatient Unit (IPU)
- TE AOD Treatment Team
- TE Memory
- TE Mental Health Access Team
- TE Mental Health Adult Team - Darwin
- TE Mental Health Adult Team - Palmerston
- TE Mental Health Child & Adolescent
- TE Mental Health Forensic Team
- TE Mental Health Inpatient Unit
- TE Mental Health Remote Team
- TE Oral Health Services
- TE PHC Outreach
- TE Prison Health
- TE Rural Medical Practitioners (RMPs)
- TE Sexual Assault Referral Centre (SARC)
- Top End Central PHCCs
- Top End Community Allied Health
- Top End Population Primary Health Care Urban
- Top End West Arnhem PHCCs
- Top End West PHCCs
Central Australia
- Alice Springs Clinic 34
- ASH Alcohol and Other Drugs
- ASH Allergy
- ASH Allied Health
- ASH Cardiology
- ASH Dermatology
- ASH Endocrinology
- ASH Gastroenterology
- ASH General Medicine
- ASH General Surgical
- ASH Genetics
- ASH Haematology
- ASH Hepatology
- ASH Infectious Diseases
- ASH Maxillofacial
- ASH Neurology
- ASH Neurosurgery
- ASH Obstetrics & Gynaecology
- ASH Oncology
- ASH Orthopaedics
- ASH Paediatrics
- ASH Palliative Care
- ASH Plastics
- ASH Preadmission
- ASH Radiation Oncology
- ASH Renal
- ASH Respiratory & Sleep Services
- ASH Rheumatology
- ASH Social Workers
- ASH Spinal Rehab
- ASH Urology
- ASH Vascular
- CA Memory Clinic (MS,PG)
- CA PHC Outreach
- CA PPHC Urban
- CA Sexual Assault Referral Centre (SARC)
- Community COVID Care CA
- DoH Alice Springs Correctional Centre
- Hearing Health Services CA & BR
- Medical Retrievals and Consultation Centre (MRaCC)
- Mental Health CA & BR
- PPHC Remote Outreach Consultation Centre (ROCC) CA Northern
- PPHC Remote Outreach Consultation Centre (ROCC) CA Other
- PPHC Remote Outreach Consultation Centre (ROCC) CA Southern/Central
- TB Clinic Alice Springs
Get help
NT Health uses Healthdirect Video Call video appointments.
Learn how to conduct video appointments:
Read more on the Healthdirect video call resource centre.
Contact Healthdirect for:
- technical support
- what you need to make a video call.
To provide feedback or suggestions about your experience using telehealth, email virtualcare.nthealth@nt.gov.au.
Termination of pregnancy (abortion)
Health professionals must understand their obligations under the law when initiating or performing a termination of pregnancy.
In the Northern Territory (NT) by law, health professionals must complete the online NT prescribed reporting form when initiating or performing a termination of pregnancy.
You can access the form below or continue reading about the law, reporting requirements and clinical guidelines for the termination of pregnancy in the NT.
For patient information, go to the Northern Territory Government website.
The law and termination of pregnancy
The Termination of Pregnancy Law Reform Act 2017 commenced on 1 July 2017.
In 2021 the Act was amended to make termination of pregnancy safer and easier to access.
The Termination of Pregnancy Law Reform Regulations 2017 state the direction and set penalties under the Act.
Read the Act and Regulation's:
- Termination of Pregnancy Law Reform Act (2017)
- Termination of Pregnancy Law Reform Regulations (2017)
For more information read termination of pregnancy - summary of changes PDF (460.7 KB).
Clinical guidelines for termination of pregnancy
The purpose of the NT clinical guideline is to assist healthcare professionals in providing care to patients requesting a termination of pregnancy.
Read the Northern Territory clinical guidelines for termination of pregnancy PDF (1.7 MB)
Conscientious objector
Conscientious objectors can use the referral for pregnancy services form.
You must refer the patient within 2 working days and ensure the referral doctor has capacity to assess in sufficient time.
Reporting requirements
Medical practitioners have a responsibility by law to provide information to the NT Chief Health Officer when initiating or performing a termination of pregnancy.
Information to be provided
The following information is prescribed by the regulations:
- date of birth of the woman or pregnant person
- gestational age
- date the termination was performed/ initiated
- method of termination
- region of person’s usual residence - read the factsheet regions for prescribed information reporting PDF (290.5 KB)
- full name and provider number of the suitably qualified medical practitioner performing the termination
- full name and provider number of the second suitably qualified medical practitioner consulted for post 24 week termination of pregnancy
- Aboriginal and Torres Strait Islander status of the person
- region where the termination was initiated (for early medical terminations) or performed (for surgical terminations)
- name of the facility (post 9 weeks gestation/ surgical procedure)
- whether the termination was performed or initiated in an emergency situation (under section 10 of the Act)
- confirmation that a follow-up appointment was made.
Reporting timeframes
| Method of termination | Reporting timeframes |
|---|---|
| Early medical termination | Within 28 days of the last consultation with the woman |
| Surgical termination | Within 28 days after performance of termination |
| For any other termination | Within 28 days after performance of termination |
Purpose of collecting prescribed information
The purpose of collecting this data is to ensure safety and to assist with planning future sexual and reproductive health initiatives in the NT.
Confidentiality remains a priority and the client is not identified as part of the reporting.
What happens to the reported prescribed information
The information is the responsibility of the NT Chief Health Officer and is managed by NT Health according to the same strict confidentiality requirements that apply to all other information collected for health related purposes.
Penalties
The regulations set out penalties for failure to provide prescribed information within the prescribed time. A penalty will not be incurred if a reasonable explanation can be provided.
Factsheet
This information is also provided as a factsheet. Read the termination of pregnancy prescribed information reporting requirements PDF (150.5 KB).
Contact
For questions about the prescribed information reporting requirements contact womenshealth.doh@nt.gov.au.
Patient resources and information
Resources have been created for pregnancy and termination options in the NT:
- Pregnancy options in the NT PDF (231.6 KB)
- Having a termination of pregnancy in the NT PDF (296.6 KB)
The NT Government website has further patient information, go to the Northern Territory Government website.
Translations
Translations are is also available in Aboriginal languages as audio files, contact womenshealth.doh@nt.gov.au.
Pregnancy options for women in the NT
- Arabic PDF (290.1 KB)
- Chinese PDF (302.5 KB)
- Greek PDF (308.4 KB)
- Punjabi PDF (356.5 KB)
- Swahili PDF (171.8 KB)
- Thai PDF (213.7 KB)
- Vietnamese PDF (244.7 KB)
Having a termination of pregnancy in the NT
Professional standards
The following websites have information about best practices for termination of pregnancy:
